Assessing the New Federalism is a multiyear Urban Institute project designed to analyze the devolution of responsibility for social programs from the federal government to the states. It focuses primarily on health care, income security, employment and training programs, and social services. Researchers monitor program changes and fiscal developments. Alan Weil is the project director. In collaboration with Child Trends, the project studies changes in family well-being. The project provides timely, nonpartisan information to inform public debate and to help state and local decisionmakers carry out their new responsibilities more effectively.
Key components of the project include a household survey, studies of policies in 13 states, and a database with information on all states and the District of Columbia. Publications and database are available free of charge on the Urban Institute's web site: http://www.urban.org. This paper is one in a series of discussion papers analyzing information from these and other sources.
This paper received special funding from The Robert Wood Johnson Foundation as part of the Urban Institute's Assessing the New Federalism project. The project received additional funding from The Annie E. Casey Foundation, the W.K. Kellogg Foundation, The Henry J. Kaiser Family Foundation, The Ford Foundation, The John D. and Catherine T. MacArthur Foundation, the Charles Stewart Mott Foundation, The David and Lucile Packard Foundation, The McKnight Foundation, The Commonwealth Fund, the Stuart Foundation, the Weingart Foundation, The Fund for New Jersey, The Lynde and Harry Bradley Foundation, the Joyce Foundation, and The Rockefeller Foundation.
The nonpartisan Urban Institute publishes studies, reports, and books on timely topics worthy of public consideration. The views expressed are those of the authors and should not be attributed to the Urban Institute, its trustees, or its funders.
CONTENTS
BACKGROUND ON MEDICAID PROGRAM DESIGN AND FINANCING
WAYS THAT STATES HAVE MAXIMIZED MEDICAID
MEDICAID PROGRAM EXPANSIONS
MEDICAID REVENUE EXPANSIONS
IMPLICATION OF MAXIMIZATION STRATEGIES
PROVIDER AND HEALTH PLAN PAYMENTS
PROGRAM FINANCING
STATE HEALTH CARE POLICYMAKING
CONFLICTS BETWEEN STATES AND THE FEDERAL GOVERNMENT
THE FUTURE OF MEDICAID FINANCING
APPENDIX A: ESTIMATING THE EFFECTIVE MATCHING RATE
Medicaid is the nation's major public source of financing of health insurance for low-income
families and long-term care services for the elderly and disabled. Policymakers designed
Medicaid so that both the federal government and the states share in program financing as well
as in setting major program policies. Medicaid financing rules require states to spend their own
funds to receive a federal financial match for Medicaid services, but there are no federal limits on program spending. This open-ended commitment of federal resources invites states to be
generous in designing their programs. At the same time, because states share in the costs, it
encourages states to use federal Medicaid dollars judiciously. State cost-sharing is also a way to assure federal policymakers and taxpayers that Medicaid spending is valuable because a state is willing to spend money on the program.
Within broad federal guidelines, states are given considerable discretion about specific
groups of people and services that they want to cover through their Medicaid programs. In
addition, states, to a large extent, determine how they raise their share of program costs and how much they pay Medicaid providers. While decisions about eligibility and the benefit package
have tended be less controversial, how states raise their share of Medicaid costs and provider
payment has been an area of federal-state conflict, especially over the past decade.
Much of the controversy surrounding provider payments and states' funding sources
centers around states figuring out ways, all allowed within Medicaid law, to claim as many
federal Medicaid dollars as possible. The practice of implementing program policies designed to
expand the federal financing role in Medicaid is commonly referred to as "Medicaid
maximization." Some forms of maximization are actively encouraged and were intended, given
the structure of the program. Others, however, are not, which sometimes has made maximization
a contentious issue. These revenue maximization strategies have brought about several changes
to the structure and character of the Medicaid program. These include increasing federal
spending with no real state match contribution; creating inequities in the distribution of Medicaid funds among states; distorting program spending; and heightening tensions between federal and state governments.
In this paper, we provide a brief background on Medicaid financing and general program
design. Then we discuss some of the maximization strategies states have used and how these
strategies may have affected the Medicaid program. We conclude with some policy issues related
to Medicaid maximization and consider options that could address state actions and their impact
on the federalist structure of the program.
Background on Medicaid Program Design and Financing
The Medicaid statute sets out basic guidelines about which populations and services
states are required to cover. Federal Medicaid guidelines also impose some limitations on how
providers are paid and how services are delivered to beneficiaries. Beyond these basics, however, Medicaid law provides states with considerable latitude in the design of their Medicaid
programs. States, for example, have the option to cover a wide range of additional populations— such as the medically needy, the working disabled, and low-income working parents. They can also elect to offer a broad range of services; states can add up to 34 optional services to their programs. Both how and how much Medicaid providers are paid is also almost entirely left up to the discretion of each state.
State policymakers thus make a range of important decisions in piecing together their
Medicaid programs: Which populations are they going to cover? What services are going to be
included in their benefit package? Should service limitations be imposed? How should care be
delivered—managed care or fee-for-service? At what level should provider reimbursement be
set? Owing to the federal promise to pay for a share of all Medicaid costs, states have an
incentive to assess opportunities for Medicaid maximization when designing their programs.
Indeed, a primary goal of the federal Medicaid match is to lower states' costs of providing
coverage to low-income residents, thereby encouraging states to undertake initiatives that they
would not have done otherwise or to go beyond what they would have done on their own. The
match rate basically "discounts" the price states would otherwise face when deciding how much to spend on health care programs for their low-income population. The federal match also makes it less attractive for states to cut Medicaid during economic downturns when need is great but state revenues are low.
The federal share of Medicaid spending is determined according to a formula—called the
Federal Medical Assistance Percentage or FMAP—under which the poorest states (based on
average per capita income) receive a higher federal matching rate. By law, a state's FMAP
cannot be lower than 50 percent or greater than 83 percent. In 2000, nine states received the
minimum 50 percent FMAP, while Mississippi had the highest match, 76 percent. Of the roughly
$206 billion spent on Medicaid in 2000, almost 57 percent ($117 billion) was from the federal
government, with the remainder from states and localities (CMS 2000).
States recognize that the federal funding available through Medicaid allows them to
finance health care for the poor with less of their own funds, and all states participate in the
program. In fact, states quickly recognized the value of Medicaid. By 1971, five years after the
program was implemented, Medicaid costs totaled $6.5 billion, more than twice initial
expenditure projections. Analysts attributed the unanticipated growth in Medicaid's early days
largely to an underestimate of the extent to which states would cover optional eligibility groups and optional services (Klemm 2000). Medicaid is now one of the largest expenditure items in most states' budgets and, in the federal budget, one of the fastest growing components.
Clearly, the structure of the match rate contains incentives that influence state behavior in
the direction of Medicaid maximization. If a state is going to provide a service to its low-income population funded with state or local dollars, it is to their benefit to include the service in its Medicaid package. Similarly, the federal-state partnership encourages states to cover people through Medicaid as opposed to local or state health programs. The match also provides incentives to pay Medicaid providers generously as it can help offset potential state or local health care outlays. For example, broad Medicaid eligibility rules and generous provider payment rates can offset state or local health expenditures for the uninsured or help cover providers' uncompensated care costs.
Recognizing the potential pressure to expand Medicaid along these various dimensions—
which can cause program costs to spiral upward—the federal government retains the right to
review and approve states' Medicaid plans and changes to those plans. Further, in some cases, if
a state wants a major exception to Medicaid eligibility, payment, or service coverage rules, the
federal government can require the state to seek a research and demonstration, freedom-ofchoice,
or a home- and community-based service waiver. Not all states, however, are inclined to
"maximize" Medicaid to the same degree. Economic resources as well as underlying population differences that affect health care needs (such as the number of uninsured residents) play important roles in determining how a state designs its Medicaid program and the extent to which it maximizes Medicaid. A state's political cultural as well as the level of sophistication and expertise among state Medicaid officials and legislators regarding the many nuances of the
Medicaid program are also very important factors.
Ways That States Have Maximized Medicaid
The structure of the federal match coupled with the program flexibility under Medicaid
has provided states both the opportunity and the incentive to leverage federal funds. Over the
years, maximization strategies have come in various forms. Some entail shifting previously state-funded health programs into Medicaid. Others involve making extra Medicaid payments to
selected health care providers with states putting up little to no real state tax dollars. All of these strategies are fully allowable under Medicaid law. Indeed, in many instances, such as expanding program eligibility and service coverage, the federal government actively encouraged states to undertake the initiatives. By contrast, some of the varied Medicaid financing strategies states have used over the years have stirred considerable debate between states and the federal government.
In this section we describe some important ways states have maximized Medicaid. We
grouped maximization strategies into two broad categories, Medicaid program expansions and
Medicaid revenue expansions. Under the former, states maximize Medicaid by expanding
eligibility and services. These efforts generally operate within the basic Medicaid principles that states get more by spending more on more or better services. Thus with program expansions a
state can choose to "maximize" federal support by operating a more generous Medicaid program. States can undertake program expansions by electing the various options allowed under the program or by seeking special Medicaid waiver.
The second group of maximization strategies is Medicaid revenue expansions. As we discuss below, these have been much more controversial compared to program expansion strategies. Under the revenue expansions, which take various forms, increased federal spending takes place with limited or no state contribution. Further, in some instances, federal Medicaid dollars that are paid do not go to cover or improve health care services or expand coverage to new populations.
Medicaid Program Expansions
Shifting of State-Funded Health Services into Medicaid. A common practice among states
has been to reconfigure state-funded services so that they are in keeping with Medicaid standards and regulations. By shifting services into Medicaid, states can get federal dollars to help pay for the services that previously had been financed just with state funds. Shifting of services into Medicaid really took hold among states in the mid- to late-1980s. Among others, Medicaid has become an important source of revenue for many public health programs, particularly maternal and child health services and home health (Coughlin et al. 1999). Another area in which states pursued Medicaid maximization is mental health care. Beginning in the mid-1980s, states
increasingly moved patients out of state psychiatric hospitals, where adults age 22 to 64 are
generally ineligible for Medicaid, into the community, where they are eligible for Medicaid
(Manderscheid et al. 2000). Likewise, over the years some states—for example, Wisconsin,
California, and Washington—have shifted state-funded home care services into Medicaid.
Moving state and locally funded school-based services is another area where states have shifted
programs into Medicaid.
Expanding Populations Served under Medicaid. More recently several states have
increased the flow of federal dollars by expanding Medicaid eligibility to populations that were
either uninsured or had been covered by state-funded programs. The vehicle by which many
states undertook this type of eligibility expansion was through the Medicaid Section 1115
demonstration waiver authority.1 Though 1115 waivers had been available for many years, prior to the early 1990s they had not been used widely, in part because of the fear among federal policymakers that program costs might increase under waivers and because states viewed the federal review process as too burdensome and lengthy. Soon after then-President Clinton assumed office in 1993, his administration allowed some new assumptions about program costs under the waiver that made it easier for some states to meet the budget neutrality provisions required by 1115 waivers (Holahan et al. 1995).2 In addition, the Clinton administration made a commitment to states to streamline the waiver process. States rapidly embraced the new flexibility: Between 1993 and 1995 alone, thirteen states received 1115 waivers. Before 1993, Arizona was the only state with a statewide 1115 waiver demonstration.
While each of the 1115 programs implemented in the mid- and late-1990s is unique, a
common feature shared by many, especially the early ones, was the expansion of coverage
beyond the traditional Medicaid eligibility categories to include the uninsured or individuals
enrolled in state-funded health programs (Holahan et al. 1995).3 Key examples of these programs include the Oregon Medicaid demonstration, which, among other things, expanded Medicaid eligibility to individuals with incomes less than 100 percent of the federal poverty level. Tennessee's TennCare waiver also included a broad eligibility expansion to uninsured individuals: When first established, TennCare was open to all uninsured persons, regardless of employment status or income level.
Using somewhat of a different approach, several states now receive federal Medicaid
matching dollars through 1115 waivers for health insurance programs that had been funded
exclusively with state dollars. Examples of such waivers include Minnesota's Prepaid Medical
Assistance Program demonstration, where the state now receives Medicaid funds to help finance
its subsidized health insurance program, MinnesotaCare. Likewise, New York under its
Partnership Plan waiver gets federal Medicaid matching funds for its general assistance
population, which it previously covered under the state and local Home Relief program.
Medicaid Revenue Expansions
Medicaid Funding of General Safety Net Programs. Some states have used the Section
1115 authority to secure new federal funds to help finance their general health care safety net
programs (Coughlin and Liska 1998). California and New York are among the states that have
used this maximization strategy. In 1995 and in 2000, Los Angeles County received 1115
waivers that provided additional federal dollars to the county health care system, on the
condition that the system be restructured to have more of an emphasis on ambulatory care (Long
and Zuckerman 1998; Zuckerman and Lutzky 2001). The initial purpose of this waiver was to
financially stabilize a system that was experiencing a serious fiscal crisis in 1995 and was
considering closing its largest public hospital and privatizing others. Despite the promise for
restructuring, the waiver was viewed by many as a "bailout" of the county health system and was reported as such in the media (American Health Line 1995). Over the seven-year waiver period, Los Angeles received more than $1 billion in federal Medicaid money. The state match required to receive these federal payments was financed with intergovernmental transfers, or IGTs (see discussion below), from Los Angeles County, so that the county was helped without any additional expenditure on the part of the state of California.
Similarly New York, as part of its Partnership Plan 1115 waiver, was granted additional
federal funds to help safety net hospitals make the transition to a more competitive marketplace. With heavy promotion by hospital union officials, over the five-year waiver, New York hospitals will get $1.25 billion in federal funds. The funds can be used for a wide range of activities including worker retraining and investing in management information systems; funds do not have to be used for direct patient services. The state was able to secure these federal funds through the budget neutrality provisions provided under the 1115 waiver authority. That is, as long as states can show that expenditures under the waiver are no more than they would have been without the waiver, then states—with federal approval—can get Medicaid matching funds.
Financing and Payment Policies. Without doubt, the most controversial Medicaid
revenue strategy has been the combination of the financing policies and payment policies that
states have used in recent years to maximize federal Medicaid matching funds. Often this type of
maximization strategy is done without spending from state general revenue. We begin with a
discussion of the financing policies, followed by one of payment policies. However, it should be
noted that to make maximization work, the financing and payment policies must work in tandem.
Financing policies aimed at maximizing Medicaid began with provider taxes and
donations, which were widely used by states beginning in the mid-1980s. Ironically, provider
taxes and donations were initially approved by the Health Care Financing Administration
(HCFA, now called the Centers for Medicaid and Medicare Services or CMS). In an effort to
afford states greater flexibility in raising Medicaid funds, HCFA issued a rule in 1985 allowing
states to use donations from private medical care providers as part of their Medicaid match. West Virginia was the first state to use provider donations for this purpose. In 1986, West Virginia, facing major fiscal problems, did not have state funds to pay hospitals for Medicaid services and thus could not draw federal Medicaid matching dollars. Hospitals helped the state by "donating" money to the state. Then the state paid back the hospitals with the donated funds, earning federal Medicaid match. Thus, by paying hospitals with donated funds, West Virginia was able to receive the federal match without, in fact, having to spend any state dollars. Although the federal dollars may not have fully covered hospitals' costs in treating Medicaid patients, the donation program allowed hospitals to receive at least partial payment.
Also in the mid-1980s, some states adopted provider tax programs, which operated along
the same principle as donation programs. Under provider tax programs, states would collect tax
revenue from providers, often hospitals, and use these funds as the state share for making
Medicaid payments, especially Medicaid disproportionate share hospital payments (see
discussion below). Typically, the payments were issued to the providers that had been taxed. So,
at the end of the transaction, the hospital was fully reimbursed for their tax contribution. In other words, providers were held harmless. Florida was the first state to establish a provider tax program in 1984.
Using provider tax and donation programs as a way to raise the state share became a
common practice among states in the early 1990s. In 1990 just six states had tax and donation
programs; by 1992, 39 states had them (Ku and Coughlin 1995). While the bulk of the provider
tax and donations programs involved hospitals, other providers including intermediate care
facilities for the mentally retarded (ICF/MRs), nursing homes, and physicians were also
sometimes involved. To deal with the rapid rise in provider tax and donation programs, Congress
enacted legislation in 1991 that essentially banned states' use of provider donations and imposed restrictions on provider taxes so that taxes now have to be a "real" assessment and providers could not be guaranteed a payback of their tax contribution. As a result of the Medicaid Voluntary Contribution and Provider-Specific Tax Amendments of 1991, states had trouble enacting provider taxes that complied with the new law.
Because of these difficulties, many states turned to intergovernmental transfer (IGTs)
programs as a way to raise their state Medicaid share. As the name implies, intergovernmental
transfers are fund exchanges among or between different levels of government, and are a
common feature in state finance. For example, a state transfer of money to a county to support
primary education constitutes an IGT. Beginning in early 1990s, many states began to use IGTs
as a way to leverage federal Medicaid dollars, and IGT programs became a variant of provider
tax and donation programs. Though IGTs in and of themselves are a legally acceptable means of
raising the state's share for Medicaid,4 they are not in keeping with the spirit of how Medicaid was to be financed: Since IGTs often do not represent a true expenditure for health care services, states are not fully financing their share of Medicaid costs as was intended.
To understand how states benefit from financing policies involving IGTs (or earlier, tax
and donation programs), we show a typical transaction in Figure 1. The transaction might begin with a state receiving $10 million in revenue—in the form of an IGT, tax, or donation—from a hospital. The state would then make a $12 million Medicaid payment back to the hospital. Assuming the state has a 50 percent federal matching rate, the state would get $6 million in federal Medicaid funds. At the end of the transaction, the provider would have netted $2 million ($12 million minus $10 million) in Medicaid payments, all from federal funds. The federal government has paid $6 million in Medicaid payments, of which $4 million went to the state where the money could be used for various purposes—health or general state expenditures. At the end of the transaction, neither the state nor the locality expended any funds; only the federal government did. That the state or locality made no financial contribution is contrary to a basic tenet of Medicaid: That is, it is a program in which the federal government and states or localities share the financial burden.
These financing policies have enormous advantages for states. Each dollar of revenue
raised—from either a tax or donation program or an IGT—could generate one to three federal Medicaid matching dollars, depending upon the state's match rate. Again, depending upon the specifics of the program, the federal dollars could be generated without the state using any of its own money.
Although many states generated revenues through provider taxes, donations, and IGTs,
states had to spend this revenue because federal Medicaid matching payments are based on
expenditures not revenues. States have used two basic payment programs to spend the revenues
generated under provider tax and donation programs and through IGTs: the Medicaid
disproportionate share hospital (DSH) program and, more recently, upper payment limit (UPL)
programs.
In an effort to maintain access to health care, in the Omnibus Reconciliation Act of 1981,
Congress mandated that states consider the special payment needs of hospitals that serve a high
proportion of Medicaid and uninsured patients. These special payments came to be known as
hospital disproportionate share or DSH payments.5 Although these payments were mandated in the early 1980s, states were initially slow to act. By 1989 only a handful of states were making DSH payments. To encourage states to make Medicaid DSH payments, Congress passed several provisions during the mid-1980s. A key provision, which was included in the Omnibus Reconciliation Act of 1986, allowed states to pay hospitals rendering high volumes of care to low-income patients rates above those paid by Medicare and exceed the so-called "upper payment limit."6
The combination of raising revenue without state expense (via provider taxes, donations
and IGTs), coupled with the ability to make virtually unlimited DSH payments was central to the
extraordinary increase in Medicaid DSH expenditures in the early 1990s. Between 1990 and
1992, DSH payments (federal and state) grew from $1.4 billion to $17.5 billion and were a major
reason for the rapid growth in overall Medicaid expenditures in early 1990s (Holahan et al. 1993; Coughlin and Liska 1997). By 1996, DSH payments accounted for 1 of every 11 dollars spent on Medicaid. The extent to which states use the DSH maximization strategy varies widely (Table 1). In 1998, for example, DSH spending accounted for 22 percent of Louisiana's total Medicaid spending and nearly 20 percent of Missouri's and South Carolina's. By contrast, DSH accounted for less than 1 percent of many states' programs spending, including Arkansas's, Nebraska's and Wisconsin's.
Importantly, some of the gross DSH payments do not represent real additional dollars to
help cover hospitals' uncompensated care costs because provider taxes or IGTs are used to pay
the state share of DSH payments. Although some of the IGTs may represent local funds that are
retained by providers and ultimately used to fund health care services, only the federal share of the gross DSH payments represents new funds to providers. However, some states retain most of
the federal share of DSH payments so that hospitals actually received little, if any, additional
Medicaid revenue under the DSH program. Further, state and local subsidies to public hospitals
may be reduced in anticipation of the inflow of federal funds and these cutbacks may offset any
new revenue received under the DSH program. A 1997 survey revealed that only about 40 percent of total DSH expenditures in that year went to help hospitals' cover their costs of caring for Medicaid and uninsured individuals (Coughlin, Ku, and Kim 2000). Thus the bulk of DSH spending in 1997 was not going to cover safety net hospitals' uncompensated care costs as was the original intent behind the special payments. Not surprisingly, as discussed below, Medicaid
DSH payments have been a highly contentious issue between the states and the federal government, and on three separate occasions Congress enacted legislation to curtail DSH spending.
More recently states have developed UPL programs as a way to draw down extra federal
matching dollars (Coughlin et al. 2000; Ku 2000; U.S. GAO 2000, 2001). These programs are
essentially a variant of the DSH program: A state makes an additional Medicaid payment (that is,
payment that is over and above regular Medicaid reimbursement) to a targeted group of
providers—such as nursing homes or hospitals—that are typically owned by a county or local government. (States generally use county and locally owned providers in UPL programs because they can make IGTs to fund the state share.) The enhanced payments are well in excess of the actual cost of medical services provided to Medicaid beneficiaries. The state claims federal
Medicaid funds for the enhanced payments and then requires the providers to give back much or
all of the enhanced payment to the state in the form of IGTs. Thus, similar to DSH financing, the state receives federal matching dollars without putting up any real state funds.
Though Medicaid law grants states broad discretion in setting provider reimbursement
levels, mentioned above, it does impose the Medicare upper payment limit where Medicaid
payments (except hospital DSH payments) can be no higher than the amount that Medicare
would have paid for the same service. Importantly, whether Medicaid payments exceed the UPL
is not determined by Medicare payment for a single procedure or even on payment for all
Medicaid services a provider renders. Rather, the UPL is based on the aggregate amount that can be paid to an entire class of providers if every provider in that class were paid the Medicare rate for all services it provided to Medicaid beneficiaries. Until 2001, when the federal government issued regulations establishing three classes of providers (see discussion below),7 there were two classes of providers—state-owned and non-state-owned. The latter class includes both local publicly owned facilities and private providers.
Prior to the new 2001 regulation, a state could thus determine its UPL for, say, nursing
homes by calculating, on a statewide basis, the difference between its total Medicaid payments to all county-owned nursing homes and private nursing homes and what Medicare would have paid.
To use the UPL maximization strategy, the state would then pay the entire difference, in
supplemental Medicaid payments, to the publicly owned nursing homes. States were allowed to
pay the full UPL difference to just the public nursing homes because, as noted in the proceeding
paragraph, public and private providers were in the same provider class for UPL determination
purposes. Given that the Medicaid payment levels historically have been considerably lower than
Medicare levels, the potential for gaining additional federal dollars through UPL arrangements
was enormous.
As an example of how an UPL program works, in figure 2 we describe Pennsylvania's nursing home program as reported by HHS's Office of the Inspector General (OIG) (Mangano 2001). On June 14, 2000, Pennsylvania paid $697.1 million in supplemental payments to 23 county nursing homes. With its 54 percent FMAP, the state received $393.3 million in federal
matching funds. On the same day, the nursing homes returned $695.6 million (of the $697.1
million in supplemental payment) to the state. At the end of the transaction, the nursing homes
had a small ($1.5 million) net gain whereas the state of Pennsylvania gained $392 million.
Further, while the federal government had paid $393.3 million in Medicaid nursing home
reimbursement, no new Medicaid services appeared to have been provided with the funds. Other
states' UPL programs highlighted in the OIG report operated along a similar vein.
Systematic information on what states do with the federal funds obtained under UPL
programs is limited. However, the 2001 report by the OIG found that in some states the federal
UPL funds are effectively "recycled" to generate additional federal Medicaid matching funds (Mangano 2001). Alabama and Pennsylvania were among the states that were cited as having
UPL programs in which the federal dollars gained were used as the state match to make
subsequent Medicaid payments and, in the process, drawing another match. In short, the state is
earning "match on the match."
While some states have had UPL programs for many years, the number of programs has
grown dramatically in recent years (Ku 2000; U.S. GAO 2000, 2001). One survey showed that in
1995 states spent $313 million on UPL programs; by 1998, states spent $1.4 billion. Two years
later, in 2000, 28 states had at least one UPL program and, nationwide, an estimated $10 billion
in Medicaid UPL expenditures were made (Mangano 2001).
Implication of Maximization Strategies
The matching rate mechanism that is central to Medicaid financing encourages states to
spend more on health care for low-income populations through Medicaid than they would have
on their own. However, Medicaid maximization strategies have implications that go beyond
merely elevating spending. These range from increasing state variation in Medicaid benefit
packages and eligibility to altering provider and health plan payments to disrupting the intended balance between federal and state payments toward program costs. With all the various options, the federal government allowed for some program variation in Medicaid. Therefore, that
differences across states exist is not a major implication of Medicaid maximization.
States have used Medicaid program maximization strategies in the areas of service coverage and eligibility in ways that have made Medicaid a bigger and more costly program, and a source of funding for many health care services that had been or could have been financed with just state and local dollars. Washington's Basic Health Plan, New York's Home Relief Program, California's In-Home Support Services, Tennessee's TennCare, and Vermont's Pharmacy
Assistance Program are all examples of existing or new programs that states run but whose
funding is dependent on federal Medicaid dollars. However, and perhaps the critical element
shaping federal attitudes in this area, the state share in the costs of adding beneficiaries or
services is generally paid for from state general funds. In this way, the federal policymakers
know that states are taxing their residents, in part, to raise their share of Medicaid program costs and, therefore, putting real dollars into this health care program. Thus these efforts represent real opportunity costs for the states; state spending on Medicaid program expansions come at the expense of state spending on other objectives, including tax cuts. This is in stark contrast to Medicaid revenue programs, where states often view the federal Medicaid match as a funding source that can be used to offset rising health care costs, the costs of non-health programs or to eliminate the need to raise taxes.
Provider and Health Plan Payments
Provider payments made through DSH and UPL programs are viewed as a central
component of Medicaid maximization. Especially for DSH payments, the development of these
programs has caused dramatic state payment differences. For example, although DSH payments
are intended to offset uncompensated costs that hospitals incur on behalf of treating Medicaid
and uninsured patients, data on variation in DSH spending (table 2) show that payments go well beyond state variation in uninsurance rates: In 1998, 17 states reported less than $100 in DSH payments per uninsured person, while 12 made payments in excess of $500 per uninsured person. In short, Medicaid DSH payments are not equitably distributed across states based on population needs. Instead, differences in Medicaid DSH primarily reflect the creativity of state policymakers and a state's willingness to engage in this form of Medicaid maximization.
Program Financing
When states have used strategies to fundamentally change the financing of Medicaid,
federal concerns developed relatively quickly—but not immediately. Through the use of IGTs, in conjunction with DSH and UPL programs, states have increased the federal share of Medicaid
program costs beyond the share dictated by the matching rate. To the extent that these practices
are used, they altered the intended balance of Medicaid dollars between the federal government
and the states as well as the distribution of federal matching dollars across the states. In turn, this affects the integrity of the federal matching rate structure that is designed to have states contribute a pre-determined share of Medicaid costs.
As mentioned, the federal government pays almost 57 percent of Medicaid program
costs. The implications of UPL programs on the effective matching rate in selected states have
been explored recently by both the Inspector General (IG) of DHHS and the General Accounting
Office (Mangano 2001; U.S. GAO 2000). In its study, the GAO concluded that the basic UPL
programs currently being used in some states "inappropriately increases federal Medicaid
payment ...and violates the integrity of Medicaid's federal/state partnership" (U.S. GAO 2000). For example, GAO reported that its 1994 analysis of a UPL program run through county nursing homes in Michigan raised the federal share of Medicaid program expenditures from 56 percent (the statutory rate) to 68 percent. A study of a similar UPL program in Pennsylvania conducted by the IG of DHHS found that the state was able to achieve a matching rate of 65 percent instead of the official rate of 54 percent. To the extent that DSH programs affect financing similarly to UPL programs, they also increase the effective matching rate.
Although it is not possible to precisely assess the impact of DSH and UPL programs
across all states with the available data, we were able to estimate the effective match rate for 23 states that were included in the DHHS Inspectors General's report and that responded to a 1998 Urban Institute survey on the Medicaid DSH program (Coughlin et al. 2000). In basic terms, we lowered the reported amount of state Medicaid spending to reflect the fact that some portion of that money was raised through IGTs and, as such, does not represent real health care spending. (The details of this estimation are discussed in Appendix A.) Table 3 shows Medicaid spending as reported by the states in claiming federal matching funds (first three columns), adjusted Medicaid spending using information on IGTs from the DHHS IG report on UPL programs and a Medicaid DSH survey (second three columns), the FMAP calculated from the reported expenditure data, and the effective FMAP calculated from the adjusted data. The last column shows the difference between the calculated and adjusted FMAP. Based on this analysis, we concluded that these 23 states were able to increase their average match rate for federal fiscal year (FFY) 2000 from approximately 56 percent based on reported Medicaid expenditures to an effective rate of 59 percent.
To understand the financial impact of this seemingly small change in the FMAP, it is
necessary to recall how the match rate affects federal spending. At a 50 percent matching rate,
for every state dollar spent the federal government spends one dollar. However, at a 56 percent
matching rate, each state dollar requires the federal government to spend $1.27 (= federal
share/(1-federal share) = 0.56/(1-0.56)). Shifting the effective matching rate to 59 percent
through the use of IGTs means that the federal government would spend $1.43 for each dollar of
state spending (rather than $1.27) financed out of general revenues. Therefore, across the 23
states for which we have relatively complete data, federal spending per dollar of state general
revenue spending, on average, was increased by about 13 percent as a result of IGT financing. In
the state of New Jersey, where our estimates suggest that the matching rate was effectively
increased from 50 to 57 percent, federal spending per dollar of state general revenue increased by almost 33 percent.
In addition to altering the effective match rate, UPL and DSH programs financed through
IGT mechanisms also obscure actual levels of program spending. A recent review of UPL
programs in 28 states conducted by the IG of DHHS showed that, as a group, spending through
these programs totaled $10.3 billion in 2000, with $5.8 billion coming from the federal
government and $4.5 billion from the states (Mangano 2001). However, if the states' share of
$4.5 billion was paid with IGTs that were ultimately returned to the local governments to use as
they pleased, then it is wrong to view these UPL payments as having increased aggregate
Medicaid spending by $10.3 billion. That would overstate aggregate program spending. In
reality, Medicaid expenditures only increased by the amount of federal outlays, or $5.8 billion
rather than $10.3 billion. The same 28 states also spent $11.3 on Medicaid DSH payments in
2000, but only $6.3 billion of this amount was derived from federal funds with $5 billion from
state funds. However, like the states' UPL programs, the vast majority of the state share for DSH was financed by IGTs or analogous mechanisms. Taken together, in 2000 the 28 states' DSH and
UPL programs recorded $21.6 billion in Medicaid spending, but actual spending—net of the
state component—may have been as little as the $12.1 billion that was the federal share.
Moreover, there is no reason to believe that all of this $12.1 billion in federal spending
was used to pay for the costs of Medicaid-covered or health-related services. Some states have
been able to increase federal payments through Medicaid UPL and DSH programs to such a
degree that they have been able to use these dollars as the state share for other Medicaid
spending—termed "recycling the match," as discussed earlier—or to direct these dollars to non-health areas of their budgets (Ku 2000; Rein 2001; U.S. DHHS OIG 2001).
State Health Care Policymaking
While difficult to fully assess, maximization has also likely affected state health care
policy and the general budget making process. The influx of federal dollars and the growing
reliance on Medicaid to fund health care programs or, in some cases, general budget items may
allow states to delay tough decisions such as raising taxes or cutting back on programs. To the
extent that states can implement new maximization strategies in the face of a downturn in overall state revenues or higher-than-expected Medicaid costs, states may be able to avoid or delay tax increases. By lowering state spending on health care, maximization can also protect spending on non-health programs.
A recent response to a budget crisis in the state of Washington, a revamped supplemental
nursing home payment system in Wisconsin, and an ongoing supplemental hospital payment
program in California are all examples of how the ability to think creatively and draw in federal dollars can influence state health care policy. During Washington state's fiscal year 2002-2003 budget debate, the legislature was facing serious financing problems as a result of growing costs in a number of health care programs (Holahan and Pohl 2002). Although significant Medicaid cutbacks were considered, the state realized that it could legally alter the way it sets the upper payment limits in its county nursing home UPL program and generate $450 million in additional federal Medicaid dollars. The state took this route and made only limited cuts in health care spending.
Similarly, in preparing its 2001-03 biennial budget, Wisconsin replaced a supplemental
payment program that was designed to cover the unreimbursed costs of only county and
municipal nursing homes with a program that applies the Medicare upper payment limit to all
nursing homes to maximize federal dollars (Bruen and Wiener 2002). The state estimated that
this could generate approximately $604 million in federal dollars between 2001 and 2003 and
that this could be used to fund the state share of future Medicaid payments. However, federal
rule changes may limit the ability of the state to continue this approach. Although other
strategies—such as raising taxes or making Medicaid cuts—were available, the UPL approach was described as being the only politically feasible option that could generate enough funds to finance the reimbursement increase.
In an even bigger effort to draw federal dollars into a state, California's Medicaid
program has used supplemental payments as part of a response to hospital complaints that its
selective hospital contracting program had enabled the state to establish payments that were too
low to adequately compensate providers (CMAC 2001). Rather than adopt a major across-the-board
change in the rates paid to all contract hospitals, California developed a more targeted
approach that cost the state nothing from its general fund revenues. The state agreed to a
supplemental payment program that paid extra amounts to contract hospitals that operated
emergency rooms and qualified for Medicaid DSH payments. The state share of these
supplemental payments was funded entirely with IGTs from county and University of California
hospitals. The program has grown from under $100 million in federal payments in state fiscal
year 1992-93 to over $650 million in state fiscal year 2000-01.
Conflicts between States and the Federal Government
Perhaps the most visible consequence of maximization is the heightened tension between
states and the federal government over the Medicaid program. Over the past decade, that tension
has brought about several pieces of federal legislation and regulation aimed at curbing
maximization, especially the DSH and UPL strategies. Mentioned earlier, federal policymakers
began to intervene in 1991 when Congress passed the Medicaid Voluntary Contribution and
Provider-Specific Tax Amendments—after the Bush administration and the National Governors'
Association reached an agreement—which sought to reform the DSH program along several
dimensions. In addition to greatly restricting the use of provider donations and taxes, the 1991
law—the first time in the program's history that a stand-alone Medicaid law was enacted—also severely limited the growth in DSH spending by imposing state DSH expenditure caps. However, the law did not attempt to impose cuts to the DSH program. It also did not address any of the underlying inequities in the DSH program across states—for example, the unevenness in DSH spending among states. Instead, it more or less "froze" the program circa 1992.
Federal concerns about the DSH program persisted. In particular, federal policymakers
wanted to regulate how payments were made to individual hospitals. A major issue was that
many states were making DSH payments that exceeded hospitals' uncompensated care costs
associated with serving the Medicaid and uninsured populations. To address this, Congress
included a provision in the Omnibus Reconciliation Act of 1993 limiting DSH payments to a
single hospital to no more than 100 percent of the unreimbursed costs of providing care to
Medicaid and uninsured patients. This limit has become known as the "hospital-specific cap."
Controversy around the DSH program again surfaced during the 1997 federal budget
debate. This time Congress undertook substantial cutbacks in federal DSH spending as part of
the Balanced Budget Act (BBA). Indeed, of the $17 billion in gross Medicaid reductions
contained in the BBA over the 1998-2002 time period, about $10 billion or 60 percent were
attributed to cuts in federal DSH payments (Schneider, Chan, and Elkin 1997). The BBA set out
state-specific DSH allotments for each year in 1998 to 2002 time period, which were lower than
what had been allowed under previous law.8
However, the BBA contained no formula for distributing federal DSH payments based on
specific criteria, e.g., in accordance with low-income uninsurance rates. Instead, the state-specific allotments, which were based on historical state DSH spending patterns, have been
described as "a classic compromise" between the House and Senate versions of the DSH
provisions (Schneider et al. 1997), sometimes reflecting a state's political influence. Under the final BBA legislation states received the higher of the DSH amounts allowed under the Senate
bill and those allowed under the House bill. An additional constraint was imposed in which no
state's federal DSH funding in any year could be reduced by more than 3.5 percent of a state's
total 1995 federal Medicaid payments. This limit helped several states including Alabama,
Connecticut, and Kansas. Further, some specific states—such as Louisiana and New Jersey— received more favorable treatment in their BBA allotments. In a separate provision, BBA also made a special exception for California: For 1998 and 1999, California's hospital-specific cap was increased from 100 percent (as mandated under OBRA 1993) to 175 percent. (In subsequent legislation, this exception was made permanent for California.) Thus while Congress as a whole was interested in cutting federal DSH expenditures, individual representatives sought to protect their states.
More recently, the federal government has turned its attention to controlling UPL
programs. In the Medicare, Medicaid, and State Child Health Insurance Program Benefits
Improvement and Protection Act (BIPA) of 2000, Congress directed the Secretary of Health and
Human Services to issue regulations that would revise Medicaid UPL policies with the aim of
limiting spending. A final regulation was issued in January 2001 which, among other things,
created aggregate upper payment limits by three types of inpatient services (hospital, nursing
facility, and intermediate care facility for the mentally retarded) and by three types of provider classes—state-owned facilities, local publicly owned facilities, and private providers. Noted earlier, previously the last two facility types—local publicly owned and private—had been grouped together for purposes of calculating the UPL, and it was this grouping that allowed states to make excess payments to locally owned providers, leveraging federal match in the process.
Importantly, the January 2001 rule created two levels of UPLs. For state facilities and
private facilities (nursing homes or hospitals), and for local publicly owned nursing homes, the
UPL is set at 100 percent of the amount that Medicare would have paid for the service. However,
in recognition of the "higher costs of ...services in public hospitals," for local publicly owned hospitals, the UPL limit was set at 150 percent. (Federal Register 2001). In other words, a state could pay a local public hospital as much as 50 percent more than what Medicare would have paid for the collective services the hospital have provided to Medicaid patients. Thus with the increased limit, more federal funds are provided to states, via their public hospitals. In sum, with the 2001 rule, the federal government took important steps in controlling UPL programs but weakened that initiative in making the 150 percent payment exception for local public hospitals.
This payment exception, which was issued in the last few days of the Clinton
administration, stirred considerable controversy among the incoming Bush appointees (Combs
and Gilroy 2001; Washington Health Beat 2001). In 2002, in an effort to "restore fiscal integrity to the Medicaid program and to reduce the opportunity for abusive funding practices," a new rule removing the 150 payment exception for public hospitals was issued (Federal Register 2002). Similar to other Medicaid financing strategies, the administration's concern was that more federal dollars were going to states technically to pay for hospital care, but with no assurances that the dollars stayed at the hospitals.
The repeal of the 2001 regulation has sparked strong reaction among state and local
officials (Pear 2002). States claim that the new rule will create significant financial hardship and aggravate their budget problems. States also claim that their efforts to provide services to
Medicaid beneficiaries and to the uninsured will be affected (Ku 2001; Pear 2002). Interestingly, in somewhat of an about face, members of Congress of both parties have also objected to the new rule.
In the BIPA of 2000, Congressional policymakers also backtracked on some of their
efforts to reduce DSH spending. As a way to offset revenue losses due to the closing of the UPL
loophole, Congress postponed the 1997 BBA DSH cuts for 2001 and 2002.9 BIPA also included DSH provisions allowing states to increase the amount of DSH payments that public hospitals could receive. Modeled after the California DSH payment exemption, beginning in 2002, all states can pay public hospitals 175 percent of uncompensated care costs rather than 100 percent as stipulated by OBRA 1993 (see above). This payment exemption is for a two-year period; California's exemption, however, is indefinite.
Thus the federal-state tug-of-war over both Medicaid UPL and DSH programs will likely
be a continuing area of conflict. Further, the battle lines have become somewhat blurred in that
Congress at one point enacted DSH spending cuts and then postponed them. Likewise, with UPL
programs, Congress passed provisions to limit spending under these programs, but now appears
to be backing away from this position and, in some cases, supporting the UPL strategy. Over
time, through the various pieces of federal legislation and regulations, the federal government
has helped to legitimize the states' Medicaid revenue strategies. Further, the back and forth
between the two layers of government reflects an important political reality of the Medicaid
program. Congress wants to be fiscally responsible and close financial loopholes. However, at
the same time, members of Congress want to protect the states that they are elected to represent.
The Future of Medicaid Financing
The structure of Medicaid, with its often vague federal rules and considerable state
flexibility, all but guarantees states will have the opportunity to maximize federal matching
funds.10 However, in considering changes that might alter financing incentives, it is important to recognize that the current system has both strengths and weaknesses depending on one's perspective. As intended, the matching rate approach encourages states to spend more than they would otherwise. At the same time, the match provides incentives for state and local officials to find financial "loopholes." With over $200 billion spent each year on Medicaid, the financial stakes are high. As discussed, states have found loopholes in Medicaid financing and have used them very effectively. In addition to driving up program costs, these types of Medicaid gaming have caused tension between federal and state policymakers. However, after both states and health care providers become accustomed to the additional federal dollars, it is very difficult for congressional policymakers—who simultaneously represent federal interests and their respective states—to eliminate the loopholes. Even with these flaws, the current federal matching system seems to encourage states to undertake health care initiatives that they may not have if they had to rely solely on state dollars.
However, some of the recent Medicaid financing arrangements raise fundamental
questions about the future of Medicaid financing. To the extent that federal policymakers view
using Medicaid for revenue maximization as a problem, are there ways to prevent states from
engaging in these strategies that alter the program's financing? Or, is the federal-state financing partnership inherently flawed? Are there ways to ensure that states and localities are financial partners in Medicaid to the degree that program rules require? More broadly, does it make sense to maintain the current structure of Medicaid or would another approach, such as federalizing the program or using a block grant, be better?
Although current financing methods have both negative and positive attributes, it seems
that some changes in the program are needed to address the conflicts that have surfaced in recent years—especially with respect to the development of UPL programs, where large payments to a range of providers are involved. As we have discussed, UPL programs, as well as other creative financing arrangements, have had important and far-reaching implications for Medicaid. Perhaps most importantly, states' actions have fundamentally changed how Medicaid is financed: To varying degrees, the bulk of states now draw down some federal matching dollars with little to no state contribution. As a result, the FMAP formula has been altered and, moreover, overall Medicaid spending has been distorted.
These creative financing arrangements raise issues not only about the shared federal-state
responsibility for Medicaid, but about whether and how the financial integrity of Medicaid can
be restored. In the past, the federal government has sought to limit these abuses through various laws or regulations. For example, when states started using DSH payments to draw down extra federal funds, Congress on several occasions during the 1990s passed legislation to bring the payments under control. While DSH expenditure growth was curtailed, the provisions did not
attempt to reshape the DSH program into one that provided subsidies for uncompensated care
built on a rational foundation. Instead, the measures allowed the program to stay largely intact
with many states drawing federal match dollars with little to no state or local contribution.
Further, over the last couple years, federal policymakers seem to be backtracking on their efforts to reform the DSH program. In short, the DSH program had become part of the Medicaid
financial landscape and was too politically difficult to undo it. In the current UPL financing
debate, a similar situation appears to be taking shape.
If federal policymakers are interested in restoring greater control over Medicaid
financing, there are several alternative approaches that could be used. One is to work within the current Medicaid program design but to reduce the degree of state discretion. Among other
things, federal policymakers could develop a new formula that would more equitably distribute
DSH funds. They could also decrease the DSH payment allowance for public hospitals from 175
percent to 100 percent of uncompensated care costs. More fundamentally, akin to the DSH law
passed in 1991, the federal government could identify specific revenue sources that they would
and would not match. For example, the federal government could no longer match expenditures
in which the state share is financed with intergovernmental transfers. This would help ensure that states are truly paying their share of program costs.
Alternatively, the federal government could assume greater financial responsibility for
Medicaid. This would mean reducing the states' contribution, increasing the federal match, and
providing greater incentives for states to finance creatively and maximize federal dollars. In
return for increased funding, the federal government would have to be given more control over
Medicaid. With this broader authority, the federal government could, for example, define more
uniformly who should be covered, what types of services should be included in the benefit
structure, and how providers should be paid. It could also eliminate or overhaul the Medicaid
DSH program.
However, if federal policymakers conclude that DSH and UPL programs financed with
IGTs cannot be eliminated or if states continue to develop new creative approaches that further
compromise the design of Medicaid financing, then solutions completely outside the current
system may be necessary. For example, Medicaid could be federalized and financed just with
federal dollars, like Medicare. It may be that the loopholes available under the current federal-state arrangement can only be closed by eliminating the financing partnership entirely. Another reason that this more radical approach might be needed is that the level of tension between federal and state policymakers over program financing has escalated under both Democratic and Republican administrations and it may be very difficult, if not impossible, to restore a sense of trust. A federalized Medicaid program would also reduce interstate variation in eligibility rules and service coverage and would promote greater horizontal equity across low-income individuals. For people in some states this might lead to a less generous program, while for others eligibility and service coverage could be expanded.
Whether or not the current federal-state partnership is overhauled in any way will be
directly related to how seriously policymakers view the problems created by the current
financing schemes. To date, most changes have not fundamentally altered states' incentives or
ability to draw down some share of federal Medicaid dollars without spending from state general
revenues. Given that Medicaid program spending is now more than $200 billion, it is likely that
the matter of what to do about Medicaid financing will remain at the center of the nation's health policy debates into the future.
References
American Health Line. 1995. "Statelines-California: L.A. County Receives Bailout from
Washington," http://nationaljournal.com, September 22.
Anton, T. J. 1997. "New Federalism and Intergovernmental Fiscal Relationships: The
Implications for Health Policy." Journal of Health Politics, Policy, and Law 22(3):691-720.
Bruen, Brian K. and Joshua M. Weiner. 2002. "Recent Changes in Health Policy for
Low-Income People in Wisconsin." Washington, D.C.: The Urban Institute's Assessing the New Federalism, State Update #25.
California Medical Assistance Commission (CMAC). 2001. Annual Report to the Legislature, Sacramento, CA.
Centers for Medicare and Medicaid Services (CMS). 2000. Financial Management
Report, FY 2000. The Center for Medicaid and State Operations.
http://www.hcfa.gov/Medicaid/ofs-64.html (Accessed April 10, 2002).
Combs, Jennifer V. and Thomas Gilroy. 2001. "CMS Still Working on UPL Rule
Eliminating Leeway for Public Hospitals, Official Says." Health Care Policy Report,
9(37):1423-5.
Coughlin, Teresa A., Stephen Zuckerman, Susan Wallin, and John Holahan. 1999. "A
Conflict of Strategies: Medicaid Managed Care and Medicaid Maximization." Health Services
Research, 34(1):281-93.
Coughlin, Teresa A., and David Liska. 1997. "The Medicaid Disproportionate Share Hospital Payment Program: Background and Issues." Urban Institute's Assessing the New Federalism Series A, No. A-14, Washington, D.C., October.
———. 1998. "Changing State and Federal Payment Policies for Medicaid
Disproportionate-Share Hospitals." Health Affairs, 17(3):118-36.
Coughlin, Teresa A., Leighton Ku, and Johnny Kim. 2000. "Reforming the Medicaid
Disproportionate Share Program in the 1990s." Health Care Financing Review, 22(2):137-57.
Federal Register. 2001. January 12, 2001. 66(9):3147-77.
Federal Register 2002. January 18, 2002. 67(13):2602-11.
Holahan, John and Mary Pohl. 2002. "States as Innovators in Low-Income Health Coverage," The Urban Institute's Assessing the New Federalism Discussion Paper 02-08, June.
Holahan, John and Mary Pohl. 2002. "Recent Changes in Health Policy for Low-Income People in Washington," The Urban Institute's Assessing the New Federalism, State Update, No.26, February.
Holahan, John, Suresh Rangarajan, and Matthew Schirmer. 1999. "Medicaid Managed
Care Rates in 1998," Health Affairs, 18(3):217-27.
Holahan, John, Teresa A. Coughlin, Leighton Ku, and Shruti Rajan. 1995. "Insuring the
Poor through Medicaid 1115 Waivers." Health Affairs, 14(1):200-17.
Holahan, John, Dianne Rowland, Judy Feder, and David Heslam. 1993. "Explaining the
Recent Growth in Medicaid Spending." Health Affairs, 12(3):178-93.
Klemm, John. 2000. "Medicaid Spending: A Brief History." Health Care Financing Review, Vol. 22: 1, pp. 105-112.
Ku , Leighton. 2000. "Limiting Abuses of Medicaid Financing: HCFA's Plan to Regulate
the Medicaid Upper Payment Limit." Center on Budget and Policy Priorities, Washington, DC,
September.
———. 2001. "Administration's Regulation to Reduce Medicaid "Upper Payment Limit" would Further Worsen State Budget Crises," Center on Budget and Policy Priorities, Washington, DC, December.
Ku, Leighton and Teresa A. Coughlin. 1995. "Medicaid Disproportionate Share and
Other Special Financing Programs." Health Care Financing Review, 16(3)27-54.
Long, Sharon and Stephen Zuckerman. 1998. "Urban Health Care in Transition:
Challenges Facing Los Angeles County," Health Care Financing Review, Vol. 20: 1.
Manderscheid, Ronald W., Joanne E. Atay, María del R. Hernández-Cartagena, Pamela Y. Edmond, Alisa Male, Albert C. E. Parker, and Hongwei Zhang. 2000. "Highlights of
Organized Mental Health Services in 1998 and Major National and State Trends." In Mental
Health, United States, 2000, edited by R.W. Manderscheid and M.J. Henderson. DHHS Pub. No.
(SMA) 01-3537. Washington, DC: Superintendent of Documents, U.S. Government Printing
Office.
Mangano, Michael F. 2001. "Review of Medicaid Enhanced Payments to Local Public
Providers and the Use of Intergovernmental Transfers." Memo from principal deputy directory
of U.S. DHHS OIG to Thomas Scully, September 11.
Pear, Robert. 2002. "Budget Would Cut Medicaid Payments." New York Times, Saturday February 3.
Rein, Lisa. 2001. "Virginia Tries Medicaid Maneuver: Federal Funds Would Help Cover
Tax Shortfall." Washington Post, November 3.
Schneider, Andy, Stephen Cha and Sam Elkin. 1997. "Overview of Medicaid DSH
Provisions in the Balanced Budget Act of 1997, P.L. 105-33." Center on Budget and Policy
Priorities, Washington, D.C., September.
U.S. Department of Health and Human Services Office of Inspector General (U.S. DHHS
OIG). 2001. "Review of Medicaid Enhanced Payments to Local Public Providers and the Use of
Intergovernmental Transfers." Washington, D.C., September.
U.S. General Accounting Office (U.S. GAO). 2000. "Medicaid: State Financing Schemes
Again Drive Up Federal Payments." GAO/T-HEHS-00-193, September.
———. 2001. "Medicaid: HCFA Reversed Its Position and Approved Additional State Financing Schemes." GAO-02-147, October.
Washington Health Beat. 2001. "A Fast-Paced Session With Straight-Talking Tom,"
editor John Reichard, October 15.
Zuckerman, Stephen and Amy Lutzky. 2001. "The Medicaid Demonstration Project for Los
Angeles County, 1995-2000: Progress, But Room For Improvement." Final Evaluation Report to
Center for Medicare and Medicaid Services, available at http://urban.org/pdfs/mdp_la_FINAL.pdf.
Notes
1 Section 1115 of the Social Security Act authorizes waivers of specified provisions of Medicaid law allowing states to test a range of policy ideas, including how the program is financed, how services are delivered, and what populations are served under the waiver.
2 One of the requirements of Section 1115 waiver programs is that they be "budget neutral." That is, over the life of the waiver, the costs of the waiver program to the federal government cannot be more that they would have been without the waiver.
3 See Holahan and Pohl (2002) for details on these waiver programs.
4 Indeed, several states have long used IGTs from local governments to help pay the state's share of Medicaid. New York, for example, requires counties to pay 20 percent of the nonfederal share of Medicaid long-term care expenses and 50 percent of the nonfederal share of all other Medicaid services.
5 The rationale behind the special payments was that hospitals that provide high volumes of care to low-income Americans often lose money as a result of low Medicaid reimbursement rates. They also lose money because these same hospitals generally render high volumes of care to indigent patients and thus had high levels of uncompensated care. In addition, hospitals with large caseloads of low-income patients frequently had low private caseloads and thus were less able to shift the cost of uncompensated care to privately insured patients.
6 As a way to limit federal Medicaid expenditures, over the years HCFA established a set of upper payment limits on the total amount it would agree to pay states for certain services. The payment limits are based on service payment allowed under the Medicare program. The payment limit is not a price to be paid for each service provided, but
rather a ceiling on total Medicaid expenses above which the federal government will not match. Further, upper payment limits are set for different classes of services (such as nursing home care, inpatient hospital services, and ICF/MRs).
7 In brief, the January 2001 UPL regulation separated local publicly owned facilities from private providers. So now the UPL is determined across a narrower range of providers.
8 The BBA contained several other important DSH provisions, including a provision requiring that DSH payments made on behalf of Medicaid beneficiaries enrolled in managed care must be paid directly to hospitals rather than managed care plans. Finally, the BBA contained some longer-term DSH spending limits which are scheduled to take effect in 2002.
9 In 2003, however, the BBA DSH cuts are scheduled to go in effect.
10 Other federal assistance programs—such as social services block grants and federal manpower programs—have experienced similar issues with states successfully leveraging federal funds or finding a loophole that allowed them to use federal dollars for unintended purposes (Anton 1997).
Tables and Figures
|
| Table 1. Medicaid DSH Expenditures by State,
1998 |
| |
| State |
Medicaid DSH Payments
(in millions) |
DSH as a Share of
Total Medicaid Spending |
|
| United States |
$14,997.6 |
8.50% |
| Alabama |
393.7 |
16.6 |
| Alaska |
15.4 |
3.9 |
| Arizona |
123.4 |
6.2 |
| Arkansas |
1.7 |
0.1 |
| California |
2,450.7 |
12.5 |
| Colorado |
174.8 |
10.3 |
| Connecticut |
370.1 |
12.7 |
| Delaware |
8.0 |
1.8 |
| District of Columbia |
32.9 |
3.6 |
| Florida |
370.5 |
5.6 |
| Georgia |
409.6 |
11.0 |
| Hawaii |
— |
0.0 |
| Idaho |
2.2 |
0.5 |
| Illinois |
269.6 |
3.8 |
| Indiana |
194.7 |
7.3 |
| Iowa |
19.8 |
1.4 |
| Kansas |
45.0 |
3.9 |
| Kentucky |
194.7 |
7.3 |
| Louisiana |
738.3 |
22.6 |
| Maine |
122.4 |
10.9 |
| Maryland |
136.0 |
4.9 |
| Massachusetts |
497.3 |
8.8 |
| Michigan |
319.3 |
5.1 |
| Minnesota |
56.3 |
1.8 |
| Mississippi |
183.9 |
10.7 |
| Missouri |
666.1 |
19.6 |
| Montana |
0.2 |
0.1 |
| Nebraska |
5.9 |
0.7 |
| Nevada |
73.6 |
13.6 |
| New Hampshire |
128.4 |
16.6 |
| New Jersey |
1,020.4 |
17.8 |
| New Mexico |
9.4 |
0.9 |
| New York |
1,860.4 |
6.6 |
| North Carolina |
354.1 |
7.5 |
| North Dakota |
1.2 |
0.3 |
| Ohio |
657.0 |
9.6 |
| Oklahoma |
22.7 |
1.6 |
| Oregon |
27.0 |
1.5 |
| Pennsylvania |
546.3 |
6.2 |
| Rhode Island |
56.0 |
5.6 |
| South Carolina |
445.7 |
18.9 |
| South Dakota |
1.1 |
0.3 |
| Tennessee |
— |
0.0 |
| Texas |
1,438.9 |
13.9 |
| Utah |
4.1 |
0.6 |
| Vermont |
22.3 |
5.2 |
| Virginia |
160.7 |
6.5 |
| Washington |
332.8 |
9.3 |
| West Virginia |
21.9 |
1.6 |
| Wisconsin |
11.2 |
0.4 |
| Wyoming |
0.1 |
0.1 |
|
| Source: Spending data are from the HCFA-64 and enrollee data from the HCFA-2082. Both enrollee and spending data are for federal fiscal year 1998. |
|
| Table 2. Medicaid DSH Expenditures per Program Enrollee and per
Uninsured by State, 1998 |
| |
| |
DSH Expenditures |
| |
|
| State |
Per Medicaid Enrollee |
Per Uninsured Person |
|
| United States |
$371.40 |
$345.35 |
| Alabama |
626.73 |
589.28 |
| Alaska |
174.79 |
132.52 |
| Arizona |
190.05 |
110.10 |
| Arkansas |
3.89 |
3.32 |
| California |
395.83 |
344.05 |
| Colorado |
503.86 |
276.19 |
| Connecticut |
919.47 |
978.69 |
| Delaware |
76.08 |
79.70 |
| District of Columbia |
236.86 |
393.33 |
| Florida |
181.57 |
134.32 |
| Georgia |
334.77 |
311.47 |
| Hawaii |
0.00 |
0.00 |
| Idaho |
18.14 |
9.38 |
| Illinois |
151.09 |
159.65 |
| Indiana |
319.04 |
272.18 |
| Iowa |
61.78 |
70.91 |
| Kansas |
182.53 |
151.51 |
| Kentucky |
297.89 |
343.93 |
| Louisiana |
1,019.89 |
847.87 |
| Maine |
625.17 |
743.95 |
| Maryland |
225.30 |
193.18 |
| Massachusetts |
521.55 |
734.89 |
| Michigan |
235.73 |
266.62 |
| Minnesota |
100.96 |
132.57 |
| Mississippi |
349.18 |
353.07 |
| Missouri |
862.07 |
1,167.42 |
| Montana |
2.36 |
1.26 |
| Nebraska |
28.17 |
34.59 |
| Nevada |
562.98 |
201.45 |
| New Hampshire |
1,305.79 |
947.65 |
| New Jersey |
1,189.42 |
818.80 |
| New Mexico |
27.71 |
22.36 |
| New York |
531.51 |
594.04 |
| North Carolina |
294.67 |
311.87 |
| North Dakota |
19.24 |
13.72 |
| Ohio |
468.52 |
530.80 |
| Oklahoma |
49.44 |
38.68 |
| Oregon |
50.32 |
57.18 |
| Pennsylvania |
317.63 |
459.31 |
| Rhode Island |
376.26 |
643.38 |
| South Carolina |
679.12 |
700.68 |
| South Dakota |
12.93 |
12.01 |
| Tennessee |
0.00 |
0.00 |
| Texas |
536.78 |
300.19 |
| Utah |
20.80 |
14.11 |
| Vermont |
169.11 |
355.43 |
| Virginia |
233.01 |
174.23 |
| Washington |
363.65 |
442.24 |
| West Virginia |
58.65 |
72.83 |
| Wisconsin |
20.77 |
20.86 |
| Wyoming |
2.39 |
1.56 |
|
| Source: Spending data are from the HCFA-64 and enrollee data from the HCFA-2082. Both enrollee and spending data are for federal fiscal year 1998. Estimates of the uninsured are derived from a 3-year merge of the Current Population Survey for 1997-1999. |
|
| Table 3 Medicaid Enhanced Payments, Total Expenditures, and Effective FMAPs, FFY 2000 |
| |
| |
Medicaid Expenditures |
Adjusted Expenditures |
Calculated FMAP |
Effective FMAP |
Difference Between Calculated and Effective FMAP |
| |
|
|
|
|
|
| State |
Total |
Federal |
State |
Total |
Federal |
State |
|
| Alabama |
$2,696.4 |
$1,877.4 |
$819.0 |
$2,557.4 |
$1,877.4 |
$680.0 |
0.6963 |
0.7341 |
0.0378 |
| Alaska |
$481.3 |
$322.8 |
$158.5 |
$473.3 |
$322.8 |
$150.5 |
0.6707 |
0.6821 |
0.0113 |
| Arkansas |
$1,579.7 |
$1,154.8 |
$424.8 |
$1,564.5 |
$1,154.8 |
$409.6 |
0.7311 |
0.7382 |
0.0071 |
| California |
$21,150.6 |
$11,002.9 |
$10,147.7 |
$19,510.4 |
$11,002.9 |
$8,507.6 |
0.5202 |
0.5639 |
0.0437 |
| Georgia |
$4,321.2 |
$2,592.5 |
$1,728.7 |
$3,890.2 |
$2,592.5 |
$1,297.7 |
0.5999 |
0.6664 |
0.0665 |
| Illinois |
$7,487.7 |
$3,754.3 |
$3,733.4 |
$6,751.3 |
$3,754.3 |
$2,997.1 |
0.5014 |
0.5561 |
0.0547 |
| Indiana |
$3,470.0 |
$2,145.2 |
$1,324.8 |
$3,191.6 |
$2,145.2 |
$1,046.4 |
0.6182 |
0.6721 |
0.0539 |
| Iowa |
$1,637.9 |
$1,034.3 |
$603.7 |
$1,563.3 |
$1,034.3 |
$529.1 |
0.6314 |
0.6616 |
0.0301 |
| Kansas |
$1,410.8 |
$847.7 |
$563.0 |
$1,359.0 |
$847.7 |
$511.2 |
0.6009 |
0.6238 |
0.0229 |
| Louisiana |
$3,443.3 |
$2,422.7 |
$1,020.6 |
$3,241.3 |
$2,422.7 |
$818.6 |
0.7036 |
0.7474 |
0.0438 |
| Minnesota |
$3,322.3 |
$1,717.4 |
$1,604.9 |
$3,317.8 |
$1,717.4 |
$1,600.4 |
0.5169 |
0.5176 |
0.0007 |
| Missouri |
$3,939.5 |
$2,386.1 |
$1,553.3 |
$3,708.7 |
$2,386.1 |
$1,322.6 |
0.6057 |
0.6434 |
0.0377 |
| Montana |
$450.2 |
$335.4 |
$114.9 |
$449.9 |
$335.4 |
$114.6 |
0.7449 |
0.7454 |
0.0005 |
| New Jersey |
$6,069.8 |
$3,038.5 |
$3,031.4 |
$5,345.0 |
$3,038.5 |
$2,306.5 |
0.5006 |
0.5685 |
0.0679 |
| New York |
$30,186.3 |
$15,124.3 |
$15,062.0 |
$28,611.2 |
$15,124.3 |
$13,486.9 |
0.501 |
0.5286 |
0.0276 |
| North Carolina |
$5,464.9 |
$3,421.1 |
$2,043.8 |
$5,209.9 |
$3,421.1 |
$1,788.8 |
0.626 |
0.6566 |
0.0306 |
| North Dakota |
$428.7 |
$304.2 |
$124.4 |
$417.8 |
$304.2 |
$113.5 |
0.7097 |
0.7282 |
0.0185 |
| Oregon |
$2,110.8 |
$1,275.2 |
$835.7 |
$2,076.6 |
$1,275.2 |
$801.5 |
0.6041 |
0.6141 |
0.0099 |
| South Carolina |
$2,664.6 |
$1,869.2 |
$795.4 |
$2,533.4 |
$1,869.2 |
$664.2 |
0.7015 |
0.7378 |
0.0363 |
| South Dakota |
$395.7 |
$281.2 |
$114.5 |
$386.4 |
$281.2 |
$105.2 |
0.7106 |
0.7277 |
0.0171 |
| Tennessee |
$4,941.6 |
$3,122.7 |
$1,818.9 |
$4,799.2 |
$3,122.7 |
$1,676.5 |
0.6319 |
0.6507 |
0.0188 |
| Washington |
$3,962.5 |
$2,062.7 |
$1,899.8 |
$3,750.5 |
$2,062.7 |
$1,687.8 |
0.5206 |
0.55 |
0.0294 |
| Wisconsin |
$3,266.9 |
$1,923.4 |
$1,343.5 |
$3,193.3 |
$1,923.4 |
$1,269.9 |
0.5888 |
0.6023 |
0.0136 |
| |
| Total |
$114,882.5 |
$64,015.9 |
$50,866.6 |
$107,902.0 |
$64,015.9 |
$43,886.1 |
0.5625 |
0.5933 |
0.0307 |
|
| Source: Urban Institute estimates based on data from HCFA-64 reports and information in Coughlin, et al. (2000) and U.S. DHHS OIG (2001). |
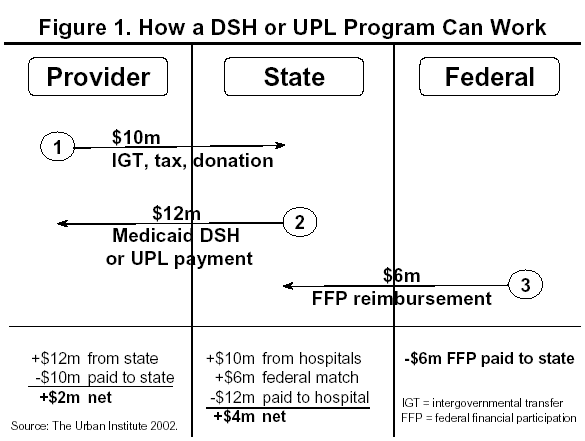
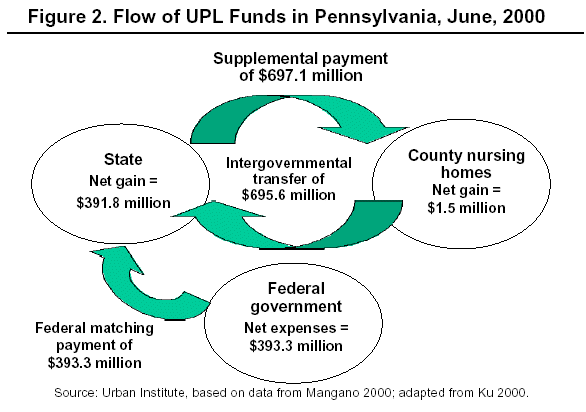
Appendix A
Estimating the Effective Match Rate
To assess the potential impact of states' use of intergovernmental transfers (IGTs),
certified public expenditures (CPEs), and provider taxes to fund Medicaid DSH and UPL
programs on the Federal Medical Assistance Percentage (FMAP), we computed the FMAP under
two alternative sets of assumptions. For the first set, we assume that all of the state Medicaid
spending reported on the Financial Management Reports represent a real expenditure of state
general funds. For the second set, we account for states' use of IGT, CPEs and providers taxes to finance their DSH and UPL program and re-estimate the FMAP using state expenditures net of
these funds. By netting out IGTs, CPEs and taxes we are assuming that these financing sources
do not represent a real state outlay.
Our first FMAP calculation is based on Medicaid Financial Management Reports from
the Centers for Medicare and Medicaid Services (CMS).1 These reports are annual summaries of data from quarterly expenditure reports (Form CMS-64) submitted by states to show the distribution of Medicaid spending for the quarter being reported and corrections for previous quarters and fiscal years. From these reports, we obtain total federal and state Medicaid expenditures for medical services and disproportionate share hospital (DSH) programs for federal fiscal year (FFY) 2000. We then use these data to calculate the FMAP for each state according to the following formula:
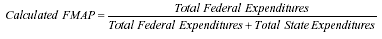
The calculated FMAP for each state based on the federal and state expenditures reported
in CMS data are shown in table 3 in the main body of this chapter. The calculated match rate often differs from the official match rate for each state printed in the Federal Register. Reasons for the discrepancies are most likely higher match rates for certain services (such as family planning) and adjustments for amounts reported for prior fiscal years when the state may have had a different match rate. We feel that the calculated FMAP is a more accurate than the published rate as it fully accounts for actual state and federal spending and adjustments to Medicaid spending.
The calculated FMAP assumes that all state Medicaid expenditures represent actual
outlays by state governments. However, expenditures financed with IGTs, CPEs, and provider
taxes generally do not represent real state outlays and our second match rate calculation—which we call the effective FMAP—addresses this issue by employing an alternative formula,
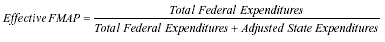
where "adjusted state expenditures" are the reported amount of state expenditures minus state Medicaid DSH and UPL expenditures funded with IGTs, CPEs, and provider taxes. The effective FMAP is shown in the second to last column in table 3.
The first step in calculating the adjusted state expenditures is to subtract the state share of DSH expenditures funded by IGTs, CPEs, and provider taxes. Because the Federal Management
Reports data only provide total state Medicaid DSH expenditures, we used DSH revenue data for
state fiscal year 1997 (collected and reported by Urban Institute researchers) as the source of the state share of DSH expenditures in each state funded by IGTs, CPEs, and provider taxes.
(Coughlin et al. 2000). Implicit in this calculation is that states' funding of DSH has not
fundamentally shifted between 1997 and 2000.
The second step in calculating adjusted state expenditures is to subtract the entire state
share of Medicaid UPL payments from state spending. A report on UPL programs released by
the Department of Health and Human Services' Office of Inspector General (OIG) in September
2001 shows that 28 states made or planned to make at least $10.3 billion in Medicaid enhanced
payments in FFY 2000, including $5.8 billion in federal funds (U.S. DHHS OIG 2001). We used
the total and federal enhanced payments for the states in the OIG report to calculate the state
share, which was then subtracted from total state Medicaid expenditures.
Ideally, we would have liked to use an adjustment for UPL that counted state Medicaid
enhanced payments financed with outlays from state general funds as actual expenditures,
particularly if the state did not recoup its general fund expenditures (for example, by requiring hospitals to return DSH funds or some portion of the UPL payment to the state).2 However, we were unable to identify an analysis of enhanced payment programs that provided sufficient data for this task. As a result, we may overestimate the amount of state funding for enhanced payments that comes from non-state sources which, in turn, results in a higher estimated effective FMAP for states that fund enhanced payments with state general fund dollars and do not recoup these funds at a point later in the process.
Table 3 in the main body of this paper shows the results of this analysis for 23 states that were included in both the Urban Institute's DSH survey and also the OIG data. Although not shown, the first adjustment reduced state Medicaid DSH expenditures for FFY 2000 (obtained from Federal Management Reports) in these 23 states from $4.5 billion to $1.0 billion. The second adjustment, which removed the entire state share of UPL payments (as reported by the
OIG) lowered reported state expenditures in these 23 states by another $3.5 billion. In total, the adjustments lowered state Medicaid expenditures in these 23 states from $50.9 billion to $43.9 billion, a 13.8 percent reduction. The effective match rate in these 23 states changed from 56 percent before the adjustment to 59 percent after the adjustment.
1 Formerly the Health Care Financing Administration (HCFA).
2 The OIG study cited earlier in this appendix found that states sometimes use UPL payments in place of DSH payments to certain hospitals, or require hospitals receiving both UPL and DSH payments to return some of the DSH payments to the state through IGTs.

